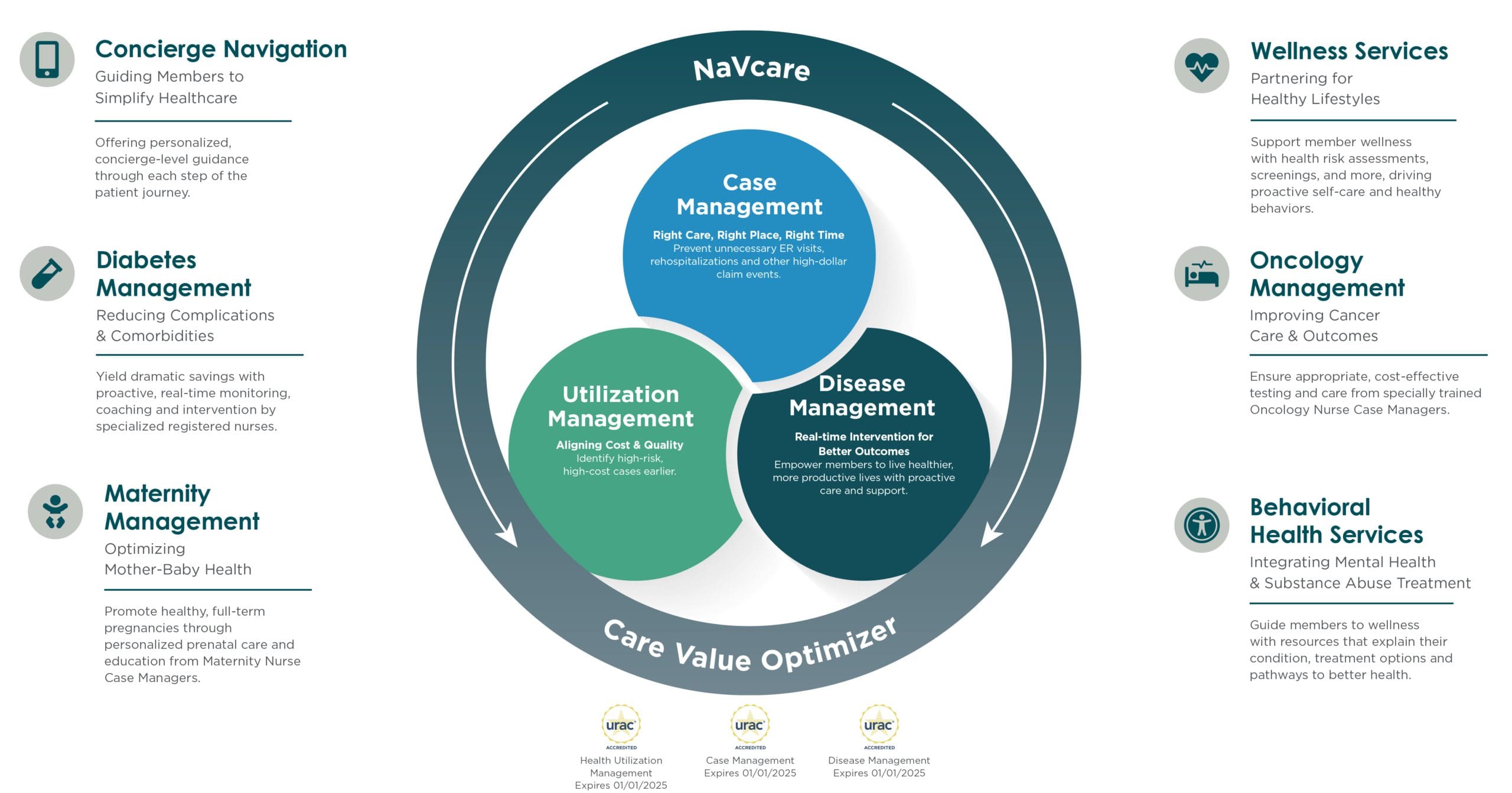
Vālenz® Health Care Management offers a suite of triple URAC-accredited care management services and targets the most appropriate levels of care at the beginning of the patient journey. Through our concierge-level member care navigation, we offer a smarter way to manage your health administrative costs while ensuring a high quality of care.
We provide your organization – and your workforce – with the right data-driven tools and care-optimized solutions for proactive health management. Position yourself to succeed in population health initiatives and medical cost management by connecting the clinical dots with Valenz.
Utilization Management
Facilitates early identification of high-risk, high-cost cases, prevents rehospitalization and reduces costs.
Case Management
Improves quality of care while steering members to network providers and maximizing cost savings.
Disease Management
Combats chronic illness, reduces costs and helps members live healthier, more productive lives.
Valenz helps build a healthy, thriving workforce by ensuring the right care in the right place at the right time – every time. We achieve this by integrating our high-value provider networks and care management services with data-driven claim and compliance solutions in our comprehensive Health Ecosystem Optimization Platform.
As the foundation of our commitment to clinical and member advocacy, Valenz engages early and often to deliver triple URAC-accredited services for case management, disease management and utilization management. We manage high-cost medical care more effectively through the Care Value Optimizer, without compromising on the quality of care.
Traditionally, a small number of claims, just 5-15% of claims, represent up to 70% of an employer’s health spend. The CVO changes this paradigm. Utilizing NaVcare, Valenz ensures a high-quality health outcome at the best price, by navigating through the myriad of care options for high-cost surgical procedures while controlling costs along the way.
First, we determine if the patient qualifies for no cost or low-cost options. Often overlooked, patients living at or below 400% of the federal poverty level can quality for full or partial elimination of bills, deductibles and copays. For those not qualifying, we offer Center of Excellence bundles for a host of high-cost procedures. Identifying high-quality ASCs and hospital centers with best-in-class outcomes, we find the right facility for the patient’s unique needs in a way that is far cheaper than traditional healthcare networks.
Ultimately, we enable your population to shift from reactive care to proactive, interactive health management – significantly reducing plan costs and driving improved health and wellness for your workforce. See what Valenz can do for Taft-Hartley Trusts, associations and public entities to drive smarter, better, faster healthcare.
NaVcare
NaVcare empowers individuals to make better health decisions while controlling costs, improving outcomes and enhancing the experience. Working one-on-one with plan members, our care navigators deliver personalized, concierge-level guidance through each step of the patient journey.
Integrated virtual care
Valenz includes seamlessly integrated virtual care services. Your plan members have 24/7 access to board-certified physician care, minimizing your exposure to unnecessary ER visits and health risks while contributing to improved patient outcomes.
Taft-Hartley Funds and Trusts
Valenz offers a suite of triple URAC-accredited care management services for all health plans, including Taft-Hartley Funds and Trusts. Lower healthcare costs require highly sophisticated and comprehensive care management strategies, which are particularly important for Taft-Hartley Funds and Trusts:
- Unionized workers often negotiate for a comprehensive package of health benefits, so Funds must find effective ways to keep healthcare contribution rates down.
- Collective bargaining allows unions to extend coverage into retirement, so understanding how to manage care and costs for this population as they age is critical.
We provide your organization – and your workforce – with the right data-driven tools and care-optimized solutions for proactive health management. Position yourself to succeed in population health initiatives and medical cost management by connecting the clinical dots with Valenz.
“I wanted to thank my nurse case manager for her advice and support through a very difficult time for me and my family. She provided great information and helped coordinate my care!”
– Jenn S., plan member